Cancer treatment is no longer limited to surgery, chemotherapy, and radiation. Over the last decade, oncology has moved toward precision medicine — therapies tailored to the biology of each patient’s tumor. Among the most promising innovations in this space are neoantigen vaccines, a personalized form of cancer immunotherapy now supported by growing clinical evidence.
At Dr Mohan Menon Cancer Center in Khar, Mumbai, patients are guided through evidence-based advancements in oncology, including emerging therapies that are shaping the future of long-term cancer control.
Understanding Neoantigen Vaccines
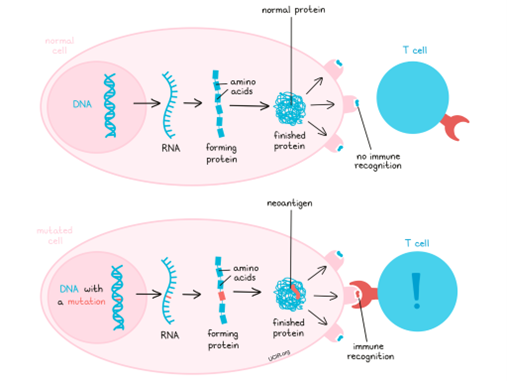
Neoantigens are mutated protein fragments that arise from genetic changes exclusive to cancer cells. Because these markers are unique to the tumor and not found in normal tissues, they provide an ideal target for immune therapies. Neoantigen vaccines work by teaching the patient’s immune system — especially T cells — to spot and attack cells displaying those mutations, while sparing healthy cells.
Unlike traditional vaccines that prevent infectious diseases like polio or measles, neoantigen vaccines are therapeutic — meaning they are used after cancer has developed, with the goal of preventing recurrence or promoting long-lasting remission.
How Neoantigen Vaccines Work: A Step-by-Step Look
- Tumour Sequencing: A biopsy of the tumour is analysed to identify genetic mutations unique to each patient’s cancer.
- Neoantigen Selection: Computational tools predict which of these mutations could most effectively stimulate the immune system.
- Vaccine Design: Using peptide-, RNA-, or DNA-based platforms, a customised vaccine is manufactured that encodes these specific neoantigens.
- Immune Activation: T cells developed to attack mutant proteins are activated by the vaccine once they are administered.
This is the reason why the neoantigen vaccines are sometimes referred to as precision immunotherapy because of such personalization.
Want to explore personalized immunotherapy options?
Schedule a consultation with a cancer specialist to understand whether advanced treatments like neoantigen vaccines may be suitable for you.
Why They Are Considered Promising
Neoantigen vaccines offer several advantages over conventional cancer treatments:
● Highly Specific Targeting: They train immune cells to only target cancer cells with the specific mutations identified in a patient’s tumour.
● Reduced Side Effects: Because healthy cells typically aren’t affected, side effects can be fewer than with traditional chemotherapy.
● Durable Immune Memory: Evidence from emerging clinical trials shows that vaccine-induced T cells may persist long after treatment, potentially preventing recurrence.
Long-Term Effectiveness: What Science Shows
Recent research paints a hopeful picture:
- In a study of pancreatic cancer, patients with an active immune response boosted successfully using an mRNA neoantigen vaccine demonstrated a long recurrence-free survival and some of the immune cells were estimated to survive more than seven years.
- Other early-phase studies in melanoma and kidney cancer show that neoantigen vaccines can produce persistent T-cell memory responses years after vaccination, which is a key factor in long-term protection.
- Combining neoantigen vaccines with checkpoint inhibitors (another immunotherapy class) has yielded deeper and more sustained responses in some patients.
While many of these findings are still in early clinical stages, they suggest that intentionally training the immune system could translate into lasting control of cancer growth.
Benefits Over Traditional Treatments
| Feature | Traditional Therapies | Neoantigen Vaccines |
| Targeting | Broad, may harm healthy cells | Highly specific to cancer mutations |
| Side Effects | Often significant | Generally milder, immune-related |
| Long-Term Protection | Limited | Potential for durable immune memory |
| Personalization | Standard schedules | Customized for each patient |
Looking for precision-based cancer care?
Connect with our oncology team today to learn more about innovative, immune-focused treatment approaches tailored to your condition.
Challenges and Limitations
Despite promising advances, there are hurdles:
- Complex Manufacturing: Personalised vaccines require time-intensive sequencing and design.
- Cost: Customisation and advanced technology can be expensive.
- Clinical Validation: Most long-term data are still from early-phase trials.
Researchers, clinicians, and biotechnology innovators continue to work on overcoming these barriers to bring neoantigen vaccines into wider clinical use.
The Future of Neoantigen Vaccines in Cancer Care

Looking forward, neoantigen vaccines could play a growing role in:
- Preventing Recurrence: T-cell memory can be long lasting and this can serve to keep cancer at bay.
- Combination Therapies: Enhanced responses when paired with checkpoint inhibitors or other immune modulators.
- Faster Turnaround Times: AI and improved sequencing methods could shorten vaccine production timelines.
This evolving landscape represents a shift toward personalised, immune-based care as a cornerstone of oncology.
